Translate this page into:
Angiomyolipoma of donor kidney: Successful transplantation and 5-year follow-up
Address for correspondence: Dr. J. Dhanapriya, Department of Nephrology, Madras Medical College and Rajiv Gandhi Government General Hospital, Chennai - 600 003, Tamil Nadu, India. E-mail: priyamdhana@yahoo.co.in
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Angiomyolipomas (AML) of the kidney are non-encapsulated benign neoplasms with the incidence of 45-80% in patients with tuberous sclerosis and 1-3% in sporadic cases. There are very few case reports in the literature in which kidneys with AML have been used for transplantation. We report here a 27-year-old female patient who received a live related renal transplant from her mother with isolated angiomyolipoma in donor kidney and on follow-up after 5 years, has stable graft function and tumor size.
Keywords
Angiomyolipoma
end-stage renal disease
graft function
kidney transplantation
tuberous sclerosis
Introduction
Bourneville in 1880 first described angiomyolipomas (AML) as a hamartoma. Renal AML is known to occur either in association with tuberous sclerosis (TSC) and lymphangiomyomatosis or sporadically. Those with asymptomatic, small sized sporadic renal AML can be considered as the potential renal donors.
Case Report
A 27-year-old lady diagnosed to have end-stage renal disease (ESRD) was started on hemodialysis. Her mother, a 55 year-old post-menopausal lady with no history of hypertension and diabetes was evaluated as the potential kidney donor. Ultrasonogram abdomen of donor showed normal sized kidneys, preserved corticomedullary differentiation and a hyperechoic lesion with uniform echogenicity in the lower pole of right kidney. Technetium-99 m renogram revealed total glomerular filtration rate 94 ml/min with distribution of left kidney – 50% (47 ml/min) and right kidney – 50% (47 ml/min). Multidetector computerized tomography (CT) showed a small non-enhancing fat attenuating nodule of 14 mm × 10 mm in the posterior cortex of the lower pole of the right kidney [Figure 1a]. Magnetic resonance imaging of brain and CT of the chest was normal. The diagnosis of sporadic AML was made after excluding syndromic causes. As there was no other donor, the transplant was done after getting consent with possible complications explained. Right donor nephrectomy was done which showed the reddish yellow mass of size 15 mm × 10 mm on the posterior surface of the lower pole [Figure 2] and graft was placed in right iliac fossa. She was discharged on day 11 with a serum creatinine of 1.2 mg/dl and was on triple immunosuppression (cyclosporine/mycophenolate mofetil/prednisolone). At 3 months, allograft biopsy was done for graft dysfunction under ultrasound guidance and showed mild acute tubular injury probably of cyclosporine toxicity. She was on regular follow-up, and periodical ultrasonogram was done for monitoring tumor size. On last follow-up at the end of 5 years, her serum creatinine was 1 mg/dl and CT abdomen showed AML of size 15 mm × 10 mm [Figure 1b].
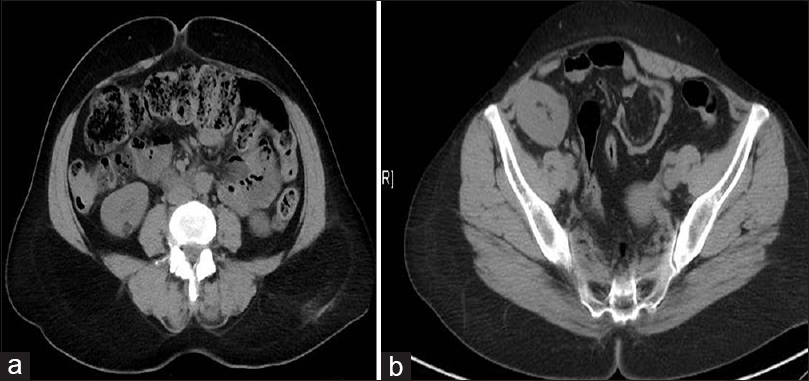
- (a) Multidetector computerized tomography showing fat attenuating nodule of size 14 mm × 10 mm in the right kidney of donor consistent with angiomyolipoma. (b) Multidetector computerized tomography done after 5 years showing with angiomyolipoma of size 15 mm × 10 mm in the renal allograft
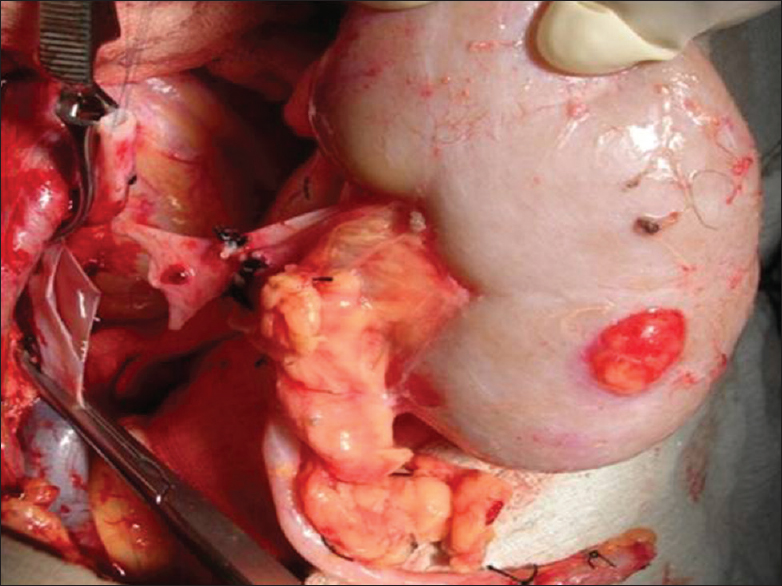
- Kidney harvested from donor showing reddish yellow mass of size 15 mm × 10 mm in the posterior surface
Discussion
Angiomyolipomas (AML) are non-encapsulated benign neoplasms composed of thickened vessels (that lack normal elastic tissue), smooth muscle and adipose tissue that arise from the mesenchymal elements of the kidney.[1] TSC is an autosomal dominant disorder characterized by the development of hamartomas in the brain, skin, heart, and kidneys.[2] In TSC, AMLs are usually small, multiple, bilateral with equal sex distribution, and their prevalence is age-related.[3] In patients with TSC, ESRD is uncommon except in massive bilateral renal involvement and associated cystic disease.[4]
Sporadic AML occur typically in middle-aged women and the tumor is often large, single, and unilateral with right kidney commonly involved.[5] The higher frequency in females is due to increased expression of estrogen and progesterone receptors in these tumors. Most of AMLs are benign and asymptomatic, but symptoms develop in 68–80% of patients when tumor size reaches 4 cm or greater. Hemorrhage is the major complication of these highly vascular tumors due to the presence of abnormal vessels and pseudoaneurysms, especially in large AMLs (>8 cm).[56] Retroperitoneal bleeding is a well-known complication of AML, sometimes leading to death (“Wunderlich syndrome”). Rarely sarcomatous changes with infiltration into surrounding tissues occur in AML.[5]
Ultrasonogram usually shows an acoustic shadow and appears homogeneous with high reflectivity due to their higher fat content. On CT, AMLs has well-defined margins, with a variable proportion of fat and soft tissue, usually with predominant fat content.[6] Small asymptomatic lesions (<4 cm) remain stable, but should be periodically evaluated, medium-sized lesions (4–8 cm) have variable behavior warranting serial imaging and large lesions(>8 cm) are associated with significant morbidity and due to the potential complications should be electively treated.[7] Surgery or embolization may be required for active hemorrhage, and mTOR inhibitors like sirolimus and everolimus therapy were found to be associated with a reduction in AML size.[8]
Rarely, renal transplantation with AML in situ or after excision either in cadaver or live related donor have been described in the literature.[91011] Lappin et al. reported 5-year follow-up of a patient who received macroscopically normal kidneys from cadaver and AML was diagnosed by biopsy.[12] Bissada et al. described a patient who underwent renal transplant after excision of AML in donor's kidney.[13] A case of isolated AML in the kidney allograft developed 3 years after transplantation and treated with partial nephrectomy of the allograft was also reported.[14]
Our patient received renal transplant with small sized AML in the graft after her consent. The potential complications in our patient - though rare - include spontaneous hemorrhage, rapid increase in tumor size with the possibility of malignant transformation later. AML was small in our donor, we chose to leave it in situ instead of excision as there was a risk of intraoperative bleeding and graft damage during the procedure. Although sirolimus and everolimus therapy was found to be beneficial in reducing AML size in nontransplant cases, we could not use these drugs due to logistic reasons. The periodic radiological evaluation was done in our patient, and it showed nonprogression of tumor size. Patient has stable graft function till last follow-up of 5 years and needs continuous monitoring.
Conclusion
Angiomyolipoma in our patient remained asymptomatic during 5-year follow-up, which is consistent with the natural history of small sized AML. We conclude that incidental and asymptomatic renal masses in a potential donor should be investigated extensively for the suitability of organ donation rather than rejecting them, in view of shortage of available donors and rising incidence of chronic kidney disease. Though additional experience with longer follow-up is needed in such patients for risk stratification and avoidance of complications.
Source of Support: Nil
Conflict of Interest: None declared.
References
- The kidney in tuberous sclerosis: Manifestations and molecular genetic mechanisms. Nephrol Dial Transplant. 1996;11(Suppl 6):34-7.
- [Google Scholar]
- Chronic renal failure and its treatment in tuberous sclerosis. Nephrol Dial Transplant. 1996;11:481-5.
- [Google Scholar]
- Changing trends in presentation, diagnosis and management of renal angiomyolipoma: Comparison of sporadic and tuberous sclerosis complex-associated forms. Urology. 2008;72:1077-82.
- [Google Scholar]
- Renal angiomyolipoma: Relationships between tumor size, aneurysm formation, and rupture. Radiology. 2002;225:78-82.
- [Google Scholar]
- Renal angiomyolipoma: Optimal treatment based on signs and symptoms. Clin Nephrol. 1998;49:281-6.
- [Google Scholar]
- Sirolimus for angiomyolipoma in tuberous sclerosis complex or lymphangioleiomyomatosis. N Engl J Med. 2008;358:140-51.
- [Google Scholar]
- Successful living related kidney transplantation despite renal angiomyolipoma in situ. J Urol. 1999;162:480-1.
- [Google Scholar]
- Renal transplantation after excision of an angiomyolipoma on living donor kidney. Prog Urol. 2004;14:205-6.
- [Google Scholar]
- Living-donor renal transplantation of grafts with incidental renal masses after ex-vivo partial nephrectomy. BJU Int. 2009;104:1655-60.
- [Google Scholar]
- Renal transplantation from living related donor after excision of angiomyolipoma of the donor kidney. J Urol. 1993;150:174-5.
- [Google Scholar]
- A rare incidence of angiomyolipoma after kidney transplantation. Iran J Kidney Dis. 2012;6:311-3.
- [Google Scholar]







