Translate this page into:
Ochoa Syndrome – Neurogenic Bladder with an Inverted Smile
Address for correspondence: Dr. Varun Govindarajan, Department of Paediatrics, Bangalore Medical College and Research Institute, Fort, K.R. Road, Bengaluru - 560 002, Karnataka, India. E-mail: varunuma@gmail.com
-
Received: ,
Accepted: ,
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Ochoa or urofacial syndrome is a rare autosomal recessive syndrome with around 150 cases reported in the medical literature comprising of neurogenic bladder and facial abnormalities, culminating in obstructive uropathy and chronic kidney disease. We report a 5-year-old boy presenting to us with Stage IV chronic kidney disease with bilateral hydroureteronephrosis secondary to chronic urinary incontinence. His peculiar facial expression with a grimace while smiling suggested the diagnosis of Ochoa syndrome. He was managed conservatively for neurogenic bladder and is under follow-up. We wish to highlight this unique syndrome and the simplicity in making this syndromic diagnosis, just by appreciating abnormal facial expressions.
Keywords
Inverted smile
neurogenic bladder
Ochoa syndrome
urofacial syndrome
Introduction
Ochoa or urofacial syndrome is a rare autosomal recessive syndrome with around 150 cases reported in the medical literature comprising of neurogenic bladder and facial abnormalities, culminating in obstructive uropathy and chronic kidney disease (CKD). In this report, we describe a 5-year-old boy with CKD secondary to neurogenic bladder, the cause was later identified as Ochoa syndrome.
Case Report
A 5-year-old boy of South Indian origin, born to nonconsanguineously married couple, was referred to the emergency room for management of hypertensive urgency. He had complaints of constant dribbling of urine noticed for 3 years of age, present throughout the day with poor stream of urine, without any urgency, fever, burning micturition, or reduced urinary output. He did not have any symptoms suggestive of hypertensive emergency. His birth and developmental history were unremarkable. He presented a history of Grade I rectal prolapse, treated conservatively, and a history of urinary tract infection (UTI) treated with antibiotics on outpatient basis, 2 years ago. The boy was underweight (12 kg) and short statured (95 cm) for his age (body mass index = 13.3), with blood pressure readings (160/90 mmHg) constantly above the 95th + 12 centiles for his age and stature. He had facial dysmorphism, with a peculiar grimace when attempting to smile [Figure 1]. He also had mild conjunctival pallor with bilateral periorbital edema. The child was developmentaly normal for age with an average IQ. External examination of the spine was normal, with no obvious sensory or motor neurological deficits noted.
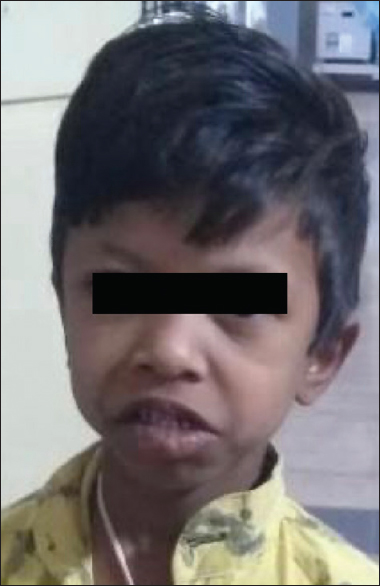
- Child with a grimace while attempting to smile (photograph taken with permission for publication)
His renal parameters were deranged (urea = 80 mg/dL, serum creatinine = 2 mg/dL) with estimated glomerular filtration rate of only 19 mL/minute/m2. His arterial blood gases revealed metabolic acidosis (pH = 7.26, HCO3− = 15.5 mmol/L, pCO2 = 33 mmHg). His abdominal ultrasound showed bilateral hydroureteronephrosis and thickened bladder wall. Diagnosis of Stage IV CKD secondary to obstructive uropathy was made, with corroborative evidence of short stature, metabolic acidosis, and normocytic normochromic anemia. Urine routine and culture ruled out UTIs. Video urodynamic study showed an initial bladder residual volume of 150 mL, detrusor pressure of 55 cmH2O, and leak patient pressure of 59 cmH2O, suggested detrusor–sphincter dyssynergia. Although the expected bladder capacity is 210 mL, the bladder started leaking at 60 mL. Micturating cystourethrogram (MCUG) showed bilateral vesicourethral reflux (VUR) with trabeculated bladder with Christmas tree pattern with multiple outpouchings and dilated posterior urethra, suggestive of neurogenic bladder [Figure 2]. Cystoscopy ruled out posterior urethral valve. Magnetic resonance imaging (MRI) spine was normal, ruling out any spinal cord lesions as cause for his neurogenic bladder. Dimercaptosuccinic acid (DMSA) scan showed bilateral renal scarring with diminished functioning of the right kidney (21%) compared with the left kidney (79%). His two-dimensional echocardiography showed mild bilateral branch pulmonary artery stenosis, although he never had experienced any cardiac symptoms till date.
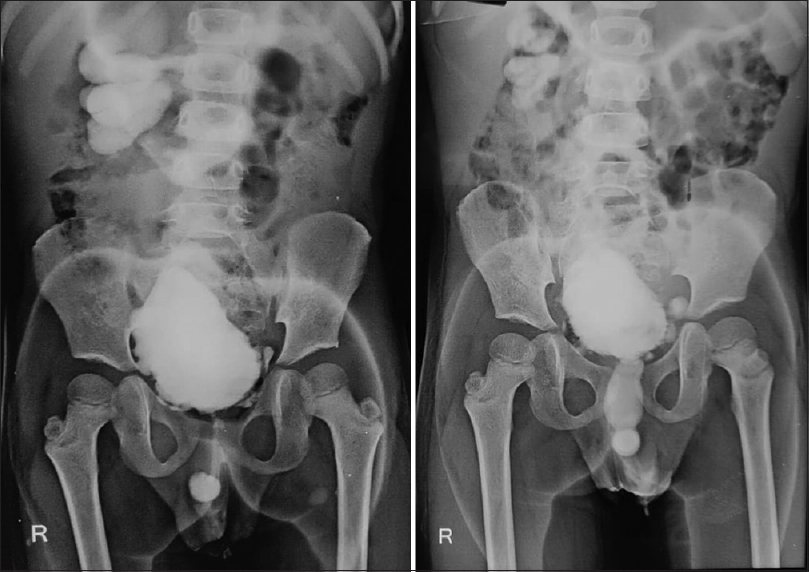
- Micturating cystourethrogram showing bilateral vesicourethral reflux with trabeculated bladder with Christmas tree pattern with multiple outpouchings and dilated posterior urethra
Nonneurogenic-type neurogenic bladder with peculiar facies of inverted smile guided us toward the diagnosis of Ochoa syndrome or urofacial syndrome (UFS). He was started on anticholinergic, oxybutynin for neurogenic bladder, and was taught clean intermittent catheterization (CIC). He required three antihypertensive drugs for the control of his hypertension. He was started on supportive therapy for CKD with calcium, iron, folic acid, sodium bicarbonate supplementation, and antibiotic prophylaxis for VUR. He is under follow-up at our center and has improving trends of renal parameters. He was also offered endocrinology consult to achieve his growth potential.
Discussion
Ochoa syndrome or UFS is an autosomal recessive congenital disorder characterized by lower urinary tract and bowel dysfunction with a typical facial expression of grimacing when attempting to smile. First described by Bernardo Ochoa in the 1960s, inverted facial smile allows early detection of this syndrome and precedes the onset of urological symptoms.[12]
It is a type of nonneurogenic neurogenic bladder, the term used to describe bladder–sphincter dysfunction in children, characterized by urinary incontinence, inefficient emptying, and recurrent UTI.[3] Bowel dysfunction is a common association. Urodynamic studies reveal detrusor–sphincter dyssynergia, responsible for urinary incontinence. Although clinical and urodynamic sequelae are identical to any neurological bladder, no neuropathological features for etiology can be demonstrated. Chronic hyperactivity of bladder and obstructive uropathy culminate in bilateral hydroureteronephrosis and CKD. Renal failure in these children is fatal by the second decade if not intervened early.
In a healthy bladder, efficient emptying is facilitated by full dilatation of outflow tract–driven neuronal nitric oxide synthase (nNOS) nerves. In UFS bladder, urinary stream is poor as the outflow fails to fully dilate and nNOS are downregulated. The destructor muscle is overactive with an abundance of aberrant nerves in bladder body secondary to bladder outlet obstruction. Mutation of HPSE2 gene, mapped to chromosome 10q23-q24 coding for heparanase 2 protein or LRIG2 gene encoding protein promoting epidermal growth factor signaling are implicated in aberrant innervations of the bladder. These genes are also implicated in facial nerve biology giving a characteristic grimace while smiling.[45] LRIG2 variants can occur in persons with non-syndromic VUR without any facial features as well.[56] Another hypothesis suggested is a subtle neurological lesion affecting the centers of micturition and laughing, which lie in close proximity in upper pons.[1] Genetic testing was not done in our child due to financial constraints.
Radiological evaluation with MCUG and MRI spine are necessary to rule out other causes for neurogenic bladder and bladder outlet obstruction. Spinal dysraphism, mostly myelodysplasia, is the most common cause for neurogenic bladder in childhood, symptoms of which may not be apparent at birth. Traumatic or neoplastic spinal lesions, sacral agenesis, and anorectal malformations can also lead to neurogenic bladder.[3] Without treatment, 60% to 80% children with neurogenic bladder develop urological problems within the first years of life, and less than 5% become continent. Posterior urethral valve (PUV) must be ruled out in all male children presenting with obstructive urinary symptoms. MRI spine was normal in our child, essentially ruling out spinal causes for neurogenic bladder, complemented by urodynamic study, MCUG, and cystoscopy, ruling out PUV. Posterior urethral dilation in our case may be due to chronic bladder sphincter spasm. Hinman syndrome, a type of nonneurogenic neurogenic bladder is a close differential of UFS caused by acquired behavioral disorder manifesting as bladder dysfunction with similar posterior urethral dilation. They are benefitted from the alleviation of psychosocial pressures.[7]
The main goals of treatment include preservation/improvement of renal function, prevention of UTI, and urinary tract deterioration. Early pediatric intervention with the institution of prophylactic therapy prevents deterioration of obstructive uropathy, by achieving a low pressure and adequate bladder capacity.[6] Restoration of balanced bladder emptying can be achieved with CIC, anticholinergics, antibiotic prophylaxis, and if needed intravesical botulinum toxin injection. Urinary diversion or bladder augmentation may be necessary in severe cases.[8]
Our case is similar to the child described by Sutay et al.[9] with a characteristic presentation of peculiar facial expression, obstructive uropathy, chronic renal failure, and associated complications, managed conservatively with CIC and anticholinergic therapy. Although a rare entity, early diagnosis and treatment can avoid significant urinary damage in these children, providing a better quality of life.
Ethics approval
Approved by Institute Ethics Board.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Can a congenital dysfunctional bladder be diagnosed from a smile.The Ochoa syndrome updated? Pediatr Nephrol. 2004;19:6-12.
- [Google Scholar]
- EAU/ESPU guidelines on the management of neurogenic bladder in children and adolescent part I diagnostics and conservative treatment. Neurourol Urodyn. 2020;39:45-57.
- [Google Scholar]
- Lrig2 and Hpse2, mutated in Urofacial syndrome, pattern nerves in the urinary bladder. Kidney Int. 2019;95:1138-52.
- [Google Scholar]
- Urofacial syndrome: A subset of neurogenic bladder dysfunction syndromes? Urology. 2011;78:911-3.
- [Google Scholar]







