Translate this page into:
70% Ethanol Lock for Management of Catheter-Related Blood-Stream Infection in Tunneled Central Venous Catheters
Corresponding author: K. Sampathkumar, Department of Nephrology, Meenakshi Mission Hospital and Research Centre, Madurai, India. E-mail: drksampath@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Sampathkumar K, Krishnapriya R, Andrew R, Ravindran S, Biju DR, Thomas C, et al. 70% Ethanol Lock for Management of Catheter-Related Blood-Stream Infection in Tunneled Central Venous Catheters. Indian J Nephrol. doi: 10.25259/IJN_714_2024
Abstract
Background
Tunneled cuffed central vein catheters (TCC) are extensively used for maintenance hemodialysis (HD). They may develop biofilms and cause catheter-related blood-stream infection (CRBSI). Commonly used antibiotic locks poorly penetrate biofilms, resulting in treatment failure and catheter removal. A potent microbicide that can penetrate biofilms is 70% ethanol. We used an ethanol lock (EL) for the treatment of CRBSI from TCC.
Materials and Methods
It is a retrospective three year cohort study. An EL was applied to catheter lumens for four hours. In the end, EL was syringed out, and catheters were relocked with heparin. This was repeated for five days. Appropriate systemic antibiotics were administered.
Results
The study group had 70 patients with CRBSI from TCC. The mean age was 50±16 years; 65% were males, and 49% had diabetic nephropathy. CRBSI rate was 2.7 per 1000 patient days. The first CBRSI episode occurred within 86 days (Interquartile range 44-176 days). Gram-negative bacteria caused 60% of infections. Catheter salvage was possible in 95% of patients. Survival analysis with log-rank test showed no difference between infected and non-infected catheters’ half-life (P = 0.42). No adverse events were seen.
Conculsion
In CRBSI treatment, 70% EL therapy with systemic antibiotics salvaged 95% of TCCs.
Keywords
Antibiotic
Central venous catheter
CRBSI
Ethanol
Hemodialysis
Introduction
Tunneled cuffed catheters (TCC) are widely used in both incident and prevalent hemodialysis (HD) patients, but less preferred than arteriovenous fistulae.1 TCC use is linked with infection risk, hospitalizations, and mortality.2 Biofilms are the primary risk of infection. They are planktonic bacterial colonies encased in an extracellular matrix coating the internal and external TCC surfaces within days of insertion.3,4 Periodic seeding of the bloodstream via biofilms, especially during HD, results in catheter-related blood-stream infections (CRBSI).5-7 CRBSI prevention currently includes universal precautions, antibiotic-impregnated catheters, or antimicrobial lock solutions. Trisodium citrate and taurolidine are becoming popular lock solutions, though cost and limited availability preclude their widespread use.8 Centers have various protocols to treat clinically or microbiologically diagnosed CRBSI. Catheter exchange using a guidewire or retention using antibiotic locks has a 60% success rate.9 Antibiotics poorly penetrate biofilms and pose colonization risk by creating drug-resistant bacteria. Recurrence rates are also significant.10 Catheter removal has the highest success rate, but creating alternate access can be challenging in vulnerable patients on maintenance HD. CRBSI treatment’s holy grail is to find a cheap and available locking solution that safely and effectively eradicates biofilms allowing continuous TCC use. Concentrated ethanol is an easily available and inexpensive bactericide and fungicide. It denatures proteins and does not risk bacterial resistance.11 In vitro studies have shown 70% ethanol to be very effective against common CRBSI-causing pathogens.12 An experimental in vitro study comparing concentrated ethanol with trisodium citrate showed that the former was more efficient at eradicating biofilms on silicone catheters.13 It can be readily formulated by any hospital pharmacy. Ethanol poses a lesser risk microbial resistance than antibiotics.14 A meta-analysis has shown concentrated EL to be a useful prophylactic agent against CBRSI for central venous catheters.15 Evidence on EL for CBRSI treatment in patients on HD is sparse.12,16 In this context, we share our experience of treating CRBSI in TCCs using 70% EL.
Materials and Methods
The study included incident patients on maintenance HD using TCC who underwent insertion between December 2020 and 2023. The control group had patients without CRBSI. It was suspected when patients experienced new onset fever (≥100.5°F) and ≥2 of the following symptoms: tachycardia, tachypnea, systolic BP <90 mmHg, or a change in mental status without any identifiable source other than the catheter. It was diagnosed when an organism was cultured from blood taken from both catheter hubs. Probable CRBSI was diagnosed in the absence of a positive blood culture. Patients were started on empiric broad-spectrum antibiotics with a glycopeptide and third-generation cephalosporine combination. These were later modified according to culture reports. A syringe was used to dilute 3.5 mL 100% medical grade ethanol with 1.5 mL sterile distilled water to make 5 mL 70% EL solution. It was prepared freshly by a clinical pharmacist every time for each patient. Following a saline flush, both the venous and arterial limbs of the catheter were filled with the appropriate volume of ethanol. It was syringed out after a four hour dwell time, flushed with saline, and followed by a heparin lock. This was repeated for five days without interrupting the dialysis schedule. If the blood culture was negative after five days and the fever resolved, it was considered a cure. However, catheter removal and systemic antifungal therapy were initiated upon fungemia diagnosis. Simultaneous clinical and bacteriological cures were the primary endpoints. The former included fever resolution with improved well-being; the latter included a negative repeat blood culture. Secondary endpoints included assessing the adverse effects of EL therapy. Patients were followed until primary TCC removal, death with functioning TCC, or December 31, 2023. Patients were excluded if primary TCC insertion was not within the study period, the removal date could not be verified, or if the patient was lost to follow-up.
We determined CRBSI rates per 1000 TCC days as per CDC recommendations. The outcome of interest was TCC removal, and we used time-to-event analysis to estimate TCC survival. Kaplan-Meir survival curve was compared between the CRBSI and non-CRBSI groups using the log-rank test. Potential predictors of TCC loss were analyzed using univariate and multivariate Cox regression. A two-sided p-value of < 0.05 was considered significant. Statistical analysis was performed using STATA v-17 software package. This retrospective analysis was approved by the local ethics committee and patient consent was waived.
Results
The study group had 101 patients: 70 developed CRBSI [Figure 1]. The mean age of the cohort was 51 years (+16), and 65% were males. As shown in Table 1, diabetes was the most common etiology for chronic kidney disease (CKD) (49%), followed by hypertension (33%) and chronic glomerulonephritis (16%). Right-sided internal jugular venous catheters measuring 19 cm were used in 89% of patients, followed by left-sided (10%) and femoral venous catheters (2%). Polyurethane (80%) and carbothane (21%) catheters were used. The symmetric tip design was used in 97 cases.
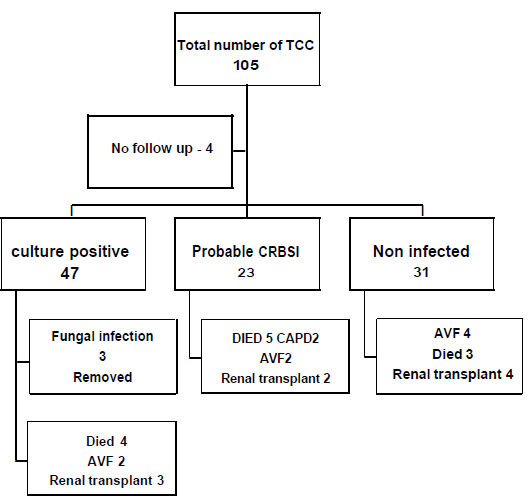
- Consort diagram. CRBSI: Catheter-related blood-stream infection, TCC: Tunneled cuffed central vein catheter, CAPD: Continuous ambulatory peritoneal dialysis, AVF: Arteriovenous fistula.
| Variable | Total n = 101 | CRBSI group N = 70 | No CRBSI N = 31 | P-value |
|---|---|---|---|---|
| Age (years) | 50.6 ± 16.1 | 50.9 ± 16.5 | 49.8 ± 15.4 | 0.75 |
| Male | 66 (65.3%) | 48 (68.6%) | 18 (58.1%) | 0.31 |
| Diabetes mellitus | 50 (49.5%) | 35 (50%) | 15 (48.4%) | 0.88 |
| Hypertension | 32 (31.7%) | 29 (41.4%) | 3 (9.7%) | 0.002 |
| Chronic glomerulonephritis | 16 (15.8%) | 4 (5.7%) | 12 (38.7%) | < 0.001 |
| Rt IJV location | 94 (93.1%) | 67 (95.7%) | 27 (87.1%) | 0.116 |
CRBSI: Catheter related blood stream infection, Rt IJV: Right side internal jugular vein
Gram-negative bacteria such as Pseudomonas, Klebsiella, Aeromonas hydrophilia, E.Coli, Acinetobacter baumannii, and Burkholderia cepacia were isolated from 60% of samples [Table 2]. Gram-positive isolates included Staph. epidermidis, S.haemolyticus, and S.hominis. Many isolates (44%) were multi-resistant to third-generation cephalosporin, aminoglycoside, and penicillin groups. Negative blood and hub cultures concluding probable CRBSI were found in 23 patients. The overall CRBSI rate in our study cohort was 2.7 per 1000 patient days. The median duration before the first CRBSI episode after TCC insertion was 86 days [Interquartile range (IQR) 44-176 days]. Systemic antibiotics were provided for appropriate durations in all cases. The four-hour dwell time was based on a study using EL in central venous catheters for preventing CRBSI in pediatric intensive care units17 EL (70%) was given for five days. Clinical and bacteriological cure with continued use of the same catheter was possible in 67 patients (95%). CRBSI did not recur after EL therapy.
| Name of the organism | Number |
|---|---|
| Klebsiella pneumoniae* | 4 |
| Pseudo. aeruginosa* | 7 |
| Escherichia coli* | 2 |
| Aeromonas hydrophilia | 2 |
| Acinetobacter baumannii* | 3 |
| Burkholderia cepacia* | 5 |
| Staph. epidermidis | 7 |
| Staph. haemolyticus | 4 |
| Staph. hominis | 1 |
| Candida | 3 |
| CONS | 2 |
| Enterococcus faecalis | 2 |
| Stenotroph. Maltophilia* | 3 |
| Enterobacter cloacae | 2 |
In Table 3, the median survival of infected TCCs (374 days) was not different from non-infected TCCs (561 days).
| Total sample | CRBSI group | No CRBSI group | P-value for difference | |
|---|---|---|---|---|
| Incidence rate of central venous catheter (CVC) removal | 1.41/1000 CVC days | 1.51/1000 CVC days | 1.06/1000 CVC days | 0.36 |
| Median CVC survival in days (IQR) | 477 (173 – 1007) | 374 (163 – 1007) | 561 (201 – 821) | 0.42 (log-rank) |
Survival of CRBSI vs. non-CRBSI catheters was not different by the log-rank test [Figure 2] (P=0.42). Table 4 shows the potential predictors of TCC loss analyzed using univariate and multivariate Cox regression. Fungal CRBSI was associated with a high catheter loss risk. TCCs were removed from all three patients who developed fungal infections. No adverse events such as catheter damage, thrombosis, septic emboli or catheter-related mortality were attributable to EL.
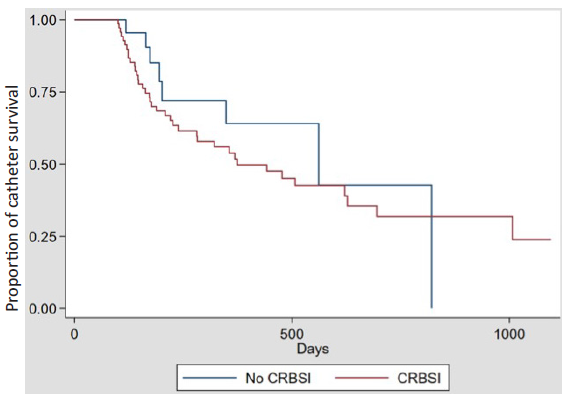
- Survival of catheter-related blood-stream infection (CRBSI) vs non-CRBSI catheters by Kaplan-Meir. log-rank test (P=0.42).
| Covariate |
Univariate HR (95% CI) |
P-value |
Multivariate HR (95% CI) |
P-value |
|---|---|---|---|---|
| Male sex | 0.82 (0.44 – 1.50) | 0.52 | 0.78 (0.42 – 1.47) | 0.45 |
| Age | 0.99 (0.98 – 1.01) | 0.92 | 0.99 (0.97 – 1.01) | 0.46 |
| Diabetes mellitus | 1.28 (0.71 – 2.32) | 0.40 | 1.47 (0.16 – 13.26) | 0.73 |
| Fungal CRBSI | 4.5 (1.9-10.5) | 0.0002* | 3.7 (1.5–8.7) | 0.0004* |
Discussion
The study assessed the EL therapy’s efficacy in the treatment of CRBSI. Earlier studies and meta-analyses only highlighted its preventive role.15 Our CRBSI diagnosis was pragmatic. We sampled equal blood volumes from both TCC ports for hemoculture and additionally from the dialysis circuit. Present symptoms and positive cultures were used to confirm CRBSI diagnosis. Quittnat Pelletier et al. showed that blood cultures from the peripheral vein, did not improve diagnosis accuracy, sensitivity, or specificity any more than a culture from the dialysis circuit or the catheter hub.18
Gram-negative bacteria were hemocultured in 60% of cases as seen in similar studies from India.16,19 This is in contrast to western observations where gram-positive bacteria were predominant. There is a notable rise in infections caused by gram-negative organisms, such as Acinetobacter and Citrobacter, which are showing growing resistance to third-generation cephalosporins and carbapenems. Antibiotic locks supplemented with systemic antibiotics salvaged only 59% of catheters.20 Our study showed infections with multiple emerging pathogens such as Aeromonas hydrophilia, Acinetobacter baumannii, Burkholderia cepacia, and Stenotrophomonas maltophilia. These were resistant to multiple antibiotics.
EL therapy combined with systemic antibiotics resulted in the successful salvage of 95% of TCCs. Twenty-three patients had probable CRBSI based on signs and symptoms with a negative hemoculture. They were also treated with EL. All recovered without need for catheter removal. There were three fungemia instances, which caused catheter removal. The catheters’ half-life with and without CRBSI was the same, as shown in the Kaplan – Meir survival graph [Figure 1]. Since the therapy cost was merely 500 INR (7 USD), it can be used as a low-cost solution. Median survival of infected catheters (374 days) was (IQR 163 – 1007 days) similar to non-infected catheters (561 days) (p=0.42). Recently, a similar study by Gang et al.,20 used EL with a shorter dwell time and antibiotics in 56 patients with CRBSI, while 17 patients received only antibiotics. Results showed a significantly higher success rate (89%) and longer catheter survival with EL than with antibiotics alone.16 Visweswaran et al. showed the possibility of fungal CRBSI eradication with EL.12
There have been no instances of catheter damage or thrombosis during the study. In-vitro studies have found that polyurethane and silicone catheters can safely be interact with 70% ethanol for up to six weeks without loss of structural integrity.21,22 In this study, the cumulative exposure was only 20 hours spread over 5 days.
Our study has the following limitations: small sample size and limited generalizability due to being a retrospective, single-center study. A control group treated with antibiotic lock therapy would have added weightage to the results.
A CRBSI episode stemming from TCCs typically manifests by the third month post-insertion. A broad bacteriological spectrum exhibiting multiple drug resistance was observed. Utilizing a 70% EL for five consecutive days alongside systemic antibiotics proved to be highly effective in managing CRBSI. In 95% of cases, the catheters remained in use without any adverse events linked to the EL. In the future, case-controlled studies that compare its effectiveness to antibiotic locks are needed.
Conflicts of interest
There are no conflicts of interest.
References
- KDOQI clinical practice guideline for vascular access: 2019 update. Am J Kidney Dis. 2020;75:S1-S164.
- [CrossRef] [PubMed] [Google Scholar]
- Infection control guidelines in hemodialysis facilities. Kidney Res Clin Pract. 2018;37:1-3.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Biofilm formation on central venous catheters: A pilot study. J Surg Res. 2022;280:123-8.
- [CrossRef] [PubMed] [Google Scholar]
- Central venous catheters and biofilms: Where do we stand in 2017? APMIS. 2017;125:365-75.
- [CrossRef] [PubMed] [Google Scholar]
- Starting hemodialysis with catheter and mortality risk: Persistent association in a competing risk analysis. J Vasc Access. 2016;17:20-8.
- [CrossRef] [PubMed] [Google Scholar]
- Catheter-related bloodstream Infections among patients on maintenance haemodialysis: A cross-sectional study at a tertiary hospital in Ghana. BMC Infect Dis. 2023;23
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Incidence of bloodstream infection in multicenter inception cohorts of hemodialysis patients. Am J Infect Control. 2004;32:155-60.
- [CrossRef] [PubMed] [Google Scholar]
- Taurolidine lock is superior to heparin lock in the prevention of catheter related bloodstream infections and occlusions. PLoS ONE. 2014;9:e111216.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Bacteremia associated with tunneled hemodialysis catheters: Outcome after attempted salvage. Clin J Am Soc Nephrol. 2009;4:1601-5.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Prevention of long-term catheter-related bloodstream infection with prophylactic antimicrobial lock solutions: Why so little use? Clinical Microbiology and Infection. 2023;29:288-290.
- [CrossRef] [PubMed] [Google Scholar]
- Reevaluation of lock solutions for central venous catheters in hemodialysis: A narrative review. Ren Fail. 2022;44:1502-19.
- [CrossRef] [Google Scholar]
- Salvage of infected tunneled hemodialysis catheters using 70% ethanol lock solution: A brief report. Hemodial Int. 2022;26:E22-6.
- [CrossRef] [PubMed] [Google Scholar]
- Eradication of microorganisms embedded in biofilm by an ethanol-based catheter lock solution. Nephrol Dial Transplant. 2009;24:3204-9.
- [CrossRef] [PubMed] [Google Scholar]
- Comparison of the effect of antibiotic-lock and ethanol-lock methods on infection rate in children with hemodialysis catheter. Am J Clin Exp Urol. 2019;7:384-90.
- [PubMed] [PubMed Central] [Google Scholar]
- Ethanol locks for the prevention of catheter related infection in patients with central venous catheter: A systematic review and meta-analysis of randomized controlled trials. PLoS One. 2019;14:e0222408.
- [PubMed] [Google Scholar]
- Hemodialysis catheter-related bloodstream infections: A single-center experience. J Nephropharmacol. 2023;12:e10475.
- [Google Scholar]
- Ethanol lock therapy for catheter-associated blood stream infections in a pediatric intensive care unit. Pediatr Crit Care Med. 2011;12:e292-6.
- [CrossRef] [PubMed] [Google Scholar]
- Evaluating approaches for the diagnosis of hemodialysis catheter-related bloodstream infections. CJASN. 2016;11:847-54.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Bacteriological profile and antibiotic resistance pattern in blood stream infection in critical care units of a tertiary care hospital in North India. Indian J Microbiol Res. 2016;3:270.
- [CrossRef] [Google Scholar]
- Role of short-dwell daily ethanol-lock therapy in the management of hemodialysis tunneled cuffed catheter-related bloodstream infection. J Vasc Access. 2024;25:1100-7.
- [CrossRef] [PubMed] [Google Scholar]
- The effects of prolonged ethanol exposure on the mechanical properties of polyurethane and silicone catheters used for intravascular access. Infect Control Hosp Epidemiol. 2005;26:708-14.
- [CrossRef] [PubMed] [Google Scholar]
- Rationale and design of the HEALTHY-CATH trial: A randomised controlled trial of Heparin versus EthAnol Lock THerapY for the prevention of catheter associated infecTion in Haemodialysis patients. BMC Nephrol. 2009;10:23.
- [CrossRef] [PubMed] [Google Scholar]







